The first sign was easy to explain away. A slight tremor in your father’s hand when he held his chai cup. You noticed it on a video call and told yourself it was nothing. He is getting older. Everyone’s hands shake a little.
Then came the call from your mother. He had fallen in the bathroom. Not badly, but enough. And the doctor had said a word that changed everything. Parkinson’s.
You did your research in the days that followed. You read about tremors and rigidity and freezing episodes. You read about the progression, the medication, and the risks. And somewhere in the middle of all that information, a quiet, specific fear took hold. How do you care for a parent with Parkinson’s when you are not there? How do you make sure the person looking after him understands what this disease actually demands?
This guide is written to answer those questions honestly and practically, so you can make decisions with clarity rather than anxiety.
What Parkinson’s Looks Like Day to Day
Parkinson’s disease is a progressive neurological condition that affects movement, balance, and, over time, a range of other functions, including speech, cognition, and emotional regulation. It is caused by the gradual loss of dopamine-producing neurons in the brain, and while it cannot be reversed, its progression can be managed significantly with the right care.
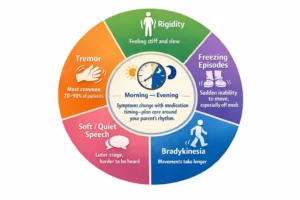
For most families, the day-to-day reality of Parkinson’s looks less like the dramatic symptoms described in medical literature and more like a series of small, accumulating challenges. Your parent may move more slowly than before. Getting out of a chair, walking to the bathroom, or buttoning a shirt may take considerably longer and require more effort than it once did. Meals may take longer. Mornings may be particularly difficult, especially before medication takes effect.
There is also the variability that makes Parkinson’s particularly hard to manage. Symptoms fluctuate throughout the day, often in relation to when medication was last taken. A parent may be relatively mobile and alert at certain hours, and significantly more limited at others. Caregivers and family members who do not understand this variability often misread it, assuming the parent is being difficult or unmotivated when they are actually in a period of genuine physical limitation.
Understanding the rhythm of your parents’ Parkinson’s, when they are typically at their best and when they need the most support, is one of the most important things a caregiver can learn.
Stage by Stage: How Care Needs Change Over Time
Parkinson’s progresses differently for every person. Some people live with mild symptoms for many years. Others experience faster progression. Most neurologists use a five-stage framework to describe the progression, though in practice the boundaries between stages are rarely clean.
In the early stages, your parent is likely still largely independent. They may need reminders about medication, some support with tasks that require fine motor control, and adjustments to the home to reduce fall risk. The caregiver’s role at this stage is more companionship and gentle monitoring than hands-on physical care.
In the middle stages, balance and coordination become more significantly affected. Freezing episodes, where the body momentarily stops responding to the brain’s instruction to move, become more common and more dangerous. Assistance with bathing, dressing, and moving around the home becomes necessary. Medication management becomes more complex. The caregiver’s role becomes more physical, more skilled, and more constant.
In the later stages, care needs become substantial. Mobility is severely limited. Swallowing difficulties may develop, creating risk during meals. Cognitive changes and dementia-like symptoms may appear. Around-the-clock care or significant caregiver presence becomes necessary, and the emotional demands on both the parent and the care team are considerable.
Knowing where your parent currently sits in this progression shapes every other decision about their care.
Home Modifications That Make a Real Difference
The home environment is especially important for a parent with Parkinson’s because the disease creates specific, predictable hazards that can be significantly reduced with targeted changes.
Falls are the most serious immediate risk. Remove all loose rugs and mats, which catch shuffling feet and cause trips. Ensure that all frequently used pathways are wide, clear, and unobstructed. Install grab bars in the bathroom, next to the toilet, and along any walls where your parent regularly steadies themselves. A raised toilet seat reduces the effort and instability involved in sitting down and standing up.
Flooring matters more than most families realise. Highly polished floors create a visual confusion that can trigger freezing in Parkinson’s patients. A consistent, matte floor surface helps the brain read the space more easily and supports more confident movement.
In the bedroom, ensure the bed is at a height that allows your parent to sit on the edge with feet flat on the floor. Bed rails on one side provide something to hold when getting up at night. A clear, lit path to the bathroom is essential because nighttime falls are disproportionately common and serious.
In the kitchen, organise frequently used items within easy reach to minimise stretching and bending. Lightweight utensils, weighted cutlery designed for tremor management, and non-slip mats under plates and bowls are small investments with meaningful daily impact.
Medication Management in Parkinson’s
Medication is not optional in Parkinson’s care. It is the foundation around which everything else is built. The primary medications used in Parkinson’s, most commonly levodopa-based treatments, work within specific time windows. When doses are missed, delayed, or taken inconsistently, the consequences are not just reduced symptom control. They can include severe freezing episodes, falls, and significant distress.
For NRI families managing care from abroad, medication adherence is one of the most important things to get right and one of the easiest things to get wrong.
A caregiver working with a Parkinson’s patient must understand the medication schedule as a non-negotiable structure around which the day is organised. They must know what each medication is for, when it should be taken, whether it should be taken with food, and what the signs of a missed or late dose look like. They should also know the name and contact number of the treating neurologist and understand when to escalate a concern.
A clearly printed medication chart, reviewed regularly by the treating doctor and kept in a visible place in the home, is a simple but essential tool. Digital pill reminders and alarm-based systems can add a layer of reliability.
Physiotherapy and Movement
Movement is medicine in Parkinson’s. Regular physiotherapy and structured daily movement have been shown to slow functional decline, improve balance, reduce freezing episodes, and support a significantly better quality of life.
In India, access to Parkinson ‘s-specialised physiotherapists varies by city, but they exist in most major urban centres and increasingly offer home visits. For families outside major cities, video-based sessions with qualified physiotherapists have become a practical and effective option.
Daily movement, even gentle and brief, matters more than occasional intensive sessions. A short walk each morning, a series of standing balance exercises, and guided stretching for rigidity in the shoulders and neck can make a meaningful difference when done consistently. A caregiver who understands the physiotherapy goals and can support and encourage daily movement, rather than discouraging activity out of an overabundance of caution, is a significant asset.
Boxing-based exercise programmes designed specifically for Parkinson’s patients, known internationally under names like Rock Steady Boxing, have also been shown to have exceptional outcomes and are beginning to appear in Indian cities. If accessible, they are worth exploring.
Emotional Support for the Parent
Parkinson’s is not only a physical condition. The emotional experience of living with it is profound and often underaddressed.
Depression affects a significant proportion of people with Parkinson’s, not only as a response to the diagnosis and its implications, but as a direct neurological consequence of the disease itself. Anxiety is also common, particularly around movement, falling, and the unpredictability of symptoms. These are not attitude problems or weaknesses. They are part of the condition and deserve to be treated with the same seriousness as the physical symptoms.
Your parent may grieve the version of themselves they used to be. They may feel embarrassed by their tremor in social situations. They may resist help not because they are being stubborn but because accepting it confronts them with something they are not ready to face.
The most important thing a caregiver and a family can offer, alongside practical support, is dignity. Speaking to your parent as a full person, not as a patient. Including them in decisions about their own care. Celebrating what they can still do rather than constantly accommodating what they cannot. These things matter more than most medical interventions.

What to Look For in a Parkinson’s Caregiver
Not every caregiver is equipped to care for a parent with Parkinson’s. The condition requires specific knowledge, specific skills, and specific personal qualities that go beyond general elder care experience.
Technically, a Parkinson’s caregiver should understand the medication regimen and its importance. They should know how to assist with mobility safely, including how to support a parent through a freezing episode without causing a fall. They should be trained in fall prevention techniques and know how to assist a person who has fallen without causing further injury. They should understand the swallowing difficulties that can develop and know how to modify food and fluid consistency appropriately.
Personally, a Parkinson’s caregiver needs patience that is genuine rather than performed. The physical pace of life with Parkinson’s is slower, and a caregiver who rushes a parent through tasks creates anxiety that worsens symptoms. They need calm in moments of distress and the emotional intelligence to distinguish a difficult day from a genuine deterioration that needs medical attention.
Ask any agency directly: what specific training has this caregiver received for Parkinson’s? What experience do they have with Parkinson’s patients specifically? The answers will separate caregivers who are genuinely equipped from those who are simply available.
Ayurvedic Approaches: What the Evidence Actually Says
Many Indian families explore Ayurvedic treatments alongside conventional Parkinson’s care, and this deserves an honest, evidence-based answer rather than either blanket dismissal or uncritical enthusiasm.
Some Ayurvedic interventions have shown genuine promise in research settings. Mucuna pruriens, a legume used in traditional medicine, contains natural levodopa and has been studied as a complementary treatment with some positive findings, though dosage and quality control remain significant variables. Ashwagandha has demonstrated some neuroprotective properties in laboratory research, though human clinical trial evidence remains limited. Abhyanga, the Ayurvedic practice of warm oil massage, may support relaxation and reduce rigidity for some patients and carries minimal risk when performed correctly.
What the evidence does not support is replacing conventional Parkinson’s medication with Ayurvedic treatments. Levodopa-based therapies remain the clinical standard for a reason. Any Ayurvedic supplementation should be discussed with the treating neurologist before it is introduced, both to assess potential interactions and to ensure that the conventional medication schedule is not disrupted.
The most sensible approach is an integrated one: conventional medicine as the foundation, with complementary approaches layered in carefully, transparently, and with medical awareness.
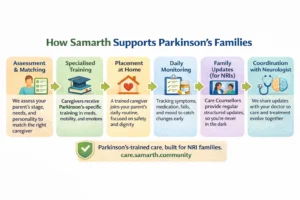
How Samarth Trains Caregivers for Parkinson’s
Parkinson’s care is one of the areas where the gap between a general caregiver and a genuinely trained one is most significant. At Samarth, we do not place a standard caregiver with a Parkinson’s patient and call it done.
Our Parkinson-trained caregivers receive condition-specific preparation that covers the neurology of the disease in accessible terms, medication management and adherence protocols, safe mobility assistance and freezing episode support, fall prevention and fall response, dietary and swallowing considerations, and the emotional dimensions of caring for someone living with a progressive condition.
Beyond training, we match caregivers to Parkinson’s patients based on temperament and pace as much as skills. A caregiver who is naturally unhurried, warm, and observant is as important as one who knows the right technique.
Our Care Counsellors maintain regular contact with families, providing structured updates on your parents’ daily functioning, any changes in symptoms, medication adherence, and the caregiver’s observations over time. For NRI children, this ongoing visibility into your parents’ day-to-day reality is not a luxury. It is the foundation of informed, confident care from a distance.
We also work alongside your parents’ neurologist, ensuring that any changes in condition are communicated to the medical team promptly and that the care plan evolves in step with the clinical picture.
Distance Does Not Mean Helplessness
A Parkinson’s diagnosis for a parent in India, received from thousands of miles away, can feel like one of the most isolating experiences an NRI child faces. The condition is serious. The care demands are real. And you cannot be there.
But the quality of care your parent receives does not depend on your physical presence. It depends on the knowledge, preparation, and support system you put in place. And that is entirely within your reach.
You have already done something important by reading this far. You are approaching this with the seriousness it deserves. The next step is making sure the person who walks through your parents’ door every morning is as prepared as you are.
Because your parent deserves care that sees them fully. Not just the diagnosis, but the person living inside it.
Looking for a caregiver who truly understands Parkinson’s?
Samarth’s trained caregivers are matched to your parent’s specific stage, needs, and personality. Every placement includes ongoing supervision, family updates, and coordination with your parents’ medical team.
Find a Parkinson’s-Trained Caregiver







