You noticed it gradually, then all at once.
Your father, who once woke before sunrise and walked five kilometres before breakfast, now sleeps until eight and tires after a short stroll. Your mother, who used to cook elaborate meals from memory, now sometimes forgets whether she has taken her afternoon medication and seems overwhelmed by decisions that would once have taken her seconds.
They seem quieter, slower, more careful. Sometimes more anxious. Sometimes more withdrawn.
And without fully meaning to, you have found yourself wondering whether they are being stubborn, or giving up, or making things harder than they need to be.
They are not. What you are observing is biology. Specific, predictable, well-documented changes in the body and brain that begin in the seventh decade of life and accelerate through the eighth and ninth. Understanding what is actually happening changes everything about how you respond to it.
This Is Not Who They Were. It Is Who They Are Becoming.
Ageing after 70 is a slow, continuous process of biological change that affects every system in the body and every function of the brain. For NRI families, that process is observed in snapshots, during visits that are too short and video calls that show a face but not a life. Changes that accumulate gradually over months can appear, from a distance, as sudden and alarming shifts.
Without a framework for understanding what is biologically normal, it is easy to misread ordinary ageing as alarming decline, or to dismiss genuine changes as simply getting older. What follows is that framework.

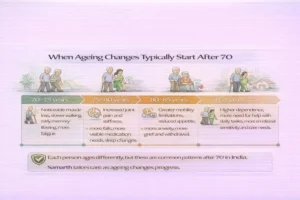
Physical Changes After 70
Mobility and Muscle
After 70, the body loses muscle mass at an accelerating rate. Muscle fibres reduce in number and size, resulting in reduced strength, slower reaction times, and significantly higher fall risk. Your parent who hesitates at the top of a staircase or walks more slowly than before is not being overly cautious. They are responding accurately to a body that is genuinely less stable than it was.
Joint cartilage also thins over time, making movement more effortful and often painful. Arthritis affects a significant proportion of people over 70 in India and contributes to the reduced mobility and morning stiffness that families frequently misread as laziness or low mood. Bone density decreases, too, meaning falls carry consequences they once did not. A fall that causes a bruise at 50 can cause a fracture at 75.
Appetite and Digestion
Many elderly parents eat less than they once did, and families often interpret this as stubbornness or depression. Often it is neither. The sense of smell and taste diminish significantly with age, directly affecting the pleasure of eating. The digestive system slows, meaning fullness arrives sooner. Saliva production decreases, making chewing and swallowing harder.
The consequences are significant. Reduced protein intake accelerates muscle loss. Inadequate hydration, also common because the sensation of thirst diminishes with age, contributes to confusion, urinary infections, and falls. A parent who is not eating or drinking well is not being difficult. They are experiencing a biological shift that needs a thoughtful response.
Sleep
Sleep architecture changes fundamentally after 70. Less time is spent in deep, restorative stages. Waking during the night becomes more common. The circadian rhythm shifts earlier, meaning many elderly people feel naturally tired in the early evening and wake very early in the morning. A parent who naps frequently and has variable energy across the day is not being self-indulgent. Their brain is managing sleep differently, and that affects mood, cognition, and immunity downstream.
Immunity
The immune system weakens with age. Infections that a younger body would resolve quickly become more serious and take longer to clear. An elderly parent who catches every seasonal illness and takes weeks to recover is not fragile by disposition. Their immune system is operating with reduced capacity, and that shapes how illness needs to be managed.
Cognitive Changes After 70
Processing Speed
The brain after 70 processes information more slowly. This is not a reduction in intelligence. It is a reduction in speed. Your parent can still reach the right conclusion or recall the memory. It simply takes longer. The pause before they answer, the deliberateness with which they approach a decision, these are expressions of normal cognitive ageing. Rushing them or presenting too much information at once consistently produces worse outcomes than giving them time.
Memory
Normal ageing affects the recall of recent events and new information. Your parent may not remember a conversation from two days ago or may struggle to retain new names. This is genuinely different from their memory for events earlier in life, which often remains remarkably intact.
What distinguishes normal memory change from the kind that warrants medical attention is pattern and progression. Forgetting where you left your keys is normal. Forgetting what keys are for is not. Forgetting a recent conversation is normal. Forgetting it happened at all, repeatedly and consistently, deserves medical attention.
Decision-Making
The part of the brain that manages planning and complex decisions changes with age. An elderly parent may find it harder to manage several things simultaneously, may become more risk-averse, and may struggle with choices that require weighing multiple options at once. This is why financial decisions and medical choices can feel overwhelming in ways that seem disproportionate. Simplifying choices, breaking decisions into smaller steps, and allowing more time are not just courteous. They are neurologically appropriate.
Emotional Changes After 70
Anxiety
Anxiety increases with age for both biological and circumstantial reasons. The brain’s capacity to regulate emotional responses changes, making anxiety easier to trigger and harder to settle. The circumstances of later life, physical vulnerability, loss of contemporaries, reduced control, create genuinely anxiety-provoking conditions. A parent who checks the door locks repeatedly or is reluctant to try new things is not simply being difficult. Their anxiety is real and deserves compassion rather than impatience.
Withdrawal and Low Mood
Emotional withdrawal can have multiple causes. Grief accumulates in later life as friends and family members are lost. Depression, which is more common in older adults and significantly underdiagnosed in India, often presents as withdrawal and reduced energy rather than overt sadness. A parent who seems less engaged and more inclined to stay home may be grieving, depressed, or lonely in a way they do not have the cultural permission to express. Each of these is a real condition deserving real attention.
Emotional Sensitivity
Many elderly parents become more emotionally sensitive with age, more easily moved, and more readily hurt by perceived criticism. This is not personality regression. It is a genuine shift in emotional regulation that comes with changes in the ageing brain. Knowing this changes how you have difficult conversations and how much weight you give to a parent’s emotional response.
How Chronic Disease Accelerates These Changes
For most elderly Indians, ageing does not happen in isolation from chronic disease. Diabetes, hypertension, heart disease, and arthritis are extremely common in this age group, and each accelerates and compounds normal ageing changes.
Diabetes affects cognition, vision, nerve health, and wound healing. Uncontrolled blood pressure increases stroke risk and contributes to cognitive decline. Arthritis compounds mobility limitations and significantly increases fall risk. Chronic pain from any source disrupts sleep, reduces appetite, and affects mood in ways that ripple across every other dimension of daily life.
This is why chronic disease management is not separate from elder care. It is central to it. A parent whose diabetes is well controlled functions significantly better across every domain than one whose diabetes is poorly managed.
What Your Parents Actually Need?
Understanding these changes reframes what good care looks like.
They need time. In conversations, decisions, and daily tasks. The ageing brain and body work more slowly, and the environment around them needs to accommodate that rather than work against it.
They need consistency. Routine reduces the cognitive load of daily life and supports better functioning. Changes to routine, however well-intentioned, create genuine disruption for an ageing brain.
They need nutrition and hydration that is actively managed. Appetite and thirst do not reliably signal need in an elderly body. Attention to what and how much a parent is eating and drinking is not excessive. It is necessary.
They need movement. Not the movement of their younger years, but appropriate, supported, daily activity that maintains muscle, supports balance, and contributes to mood and cognitive function. Encouraging stillness out of overcaution is one of the most common and consequential mistakes in elder care.
They need emotional acknowledgement. The losses of later life are real and cumulative. A parent who feels seen and companioned through those losses functions better in every other domain.
How Professional Care Addresses These Changes
A good professional caregiver does not simply assist with tasks. They understand the biology behind the behaviours they are managing.
They know that the parent who eats slowly and leaves food on the plate is experiencing diminished appetite, not being difficult. They encourage without pressuring and monitor intake over time.
They know that the parent who refuses to walk is managing genuine pain and fear of falling. They support movement safely and progressively, with attention to confidence as well as capability.
They know that the parent who seems anxious and resistant to change is not being obstructive but is managing an emotional regulation system that works differently than it once did.
At Samarth, our caregivers are trained to understand ageing as a biological process, not a personality problem. This shapes how they communicate, how they support daily activity, and how they report back to families. For NRI families, this means the person in your parents’ home every day is working with a genuine understanding of what your parents’ body and brain are going through, responding with intelligence and compassion rather than frustration.
They Have Not Changed. They Have Aged.
The parent who seems slower, more anxious, more forgetful, and less like the person you grew up with is not a diminished version of themselves. They are a person whose body and brain are moving through a process that every human being who lives long enough will experience.
Understanding that process does not make it easier to witness from a distance. But it changes what you see. Instead of stubbornness, you see a nervous system responding to genuine vulnerability. Instead of giving up, you see a body conserving energy it can no longer afford to waste.
That understanding is the beginning of care that actually fits. Care that works with your parent rather than against them. And from wherever you are in the world, building that kind of care is one of the most meaningful things you can do.
Every parent ages differently. Every care plan should too.
Samarth helps NRI families understand exactly where their parent is in their ageing journey and what support they need right now. Start with a conversation.
Understand Your Parent’s Care Needs







