You have probably made at least one decision about your parents’ care based on something you believed to be obviously true.
That forgetfulness is just part of getting old. That home is always the safest place. That family care, given with love, is better than anything a professional can offer. As long as your parent is eating and moving around, they are fine.
These beliefs are understandable. Many of them are deeply embedded in Indian cultural assumptions about ageing, family, and what it means to grow old with dignity. They are repeated across generations, reinforced by community, and rarely questioned because they feel self-evidently correct.
But many of them are wrong. And acting on them, even with the best intentions, can delay care that your parent genuinely needs, minimise conditions that deserve medical attention, and create a false sense of security that leaves real risks unaddressed.
This blog is not written to make you feel guilty about what you believed before. It is written to replace those beliefs with something more useful evidence.

Myth 1: Forgetfulness Is a Normal Part of Ageing and Nothing to Worry About
This is perhaps the most pervasive and the most consequential myth in elder care.
Some degree of memory change is indeed a normal part of ageing. Processing speed slows. Recalling recent events takes longer. New information is harder to retain. These changes are real and expected.
But forgetfulness exists on a spectrum, and not all of it is benign. When a parent repeatedly forgets conversations that happened the same day, becomes confused about time and place, loses the ability to manage familiar tasks they have performed for decades, or begins to show personality and behaviour changes alongside memory loss, these are not signs of normal ageing. They are potential signs of mild cognitive impairment or early dementia, both of which benefit significantly from early diagnosis and intervention.
The danger of the forgetfulness myth is that it functions as a reason not to act. Families reassure themselves and each other that what they are seeing is normal, months or sometimes years pass, and by the time a diagnosis is sought, the condition has progressed further than it needed to.
If you are noticing consistent, progressive memory changes in your parent, the right response is not reassurance. It is a conversation with a neurologist.
Myth 2: Home Is Always the Safest Place for an Elderly Parent
Home is familiar. Home is comfortable. Home carries decades of meaning and memory. For most elderly parents, it is genuinely the right place to be, and good care is designed to support them there for as long as possible.
But home is not inherently safe. And for an elderly parent with mobility limitations, cognitive changes, or chronic health conditions, an unmodified home can present serious and specific hazards.
Loose rugs that catch shuffling feet. Bathrooms without grab bars. Poorly lit corridors. Gas stoves left on. Medications are managed without a system. Stairs navigated alone at night.
These are not hypothetical risks. Falls are the leading cause of injury-related hospitalisation in elderly adults. Medication errors are among the most common causes of preventable health deterioration. And for parents living alone, a fall or a health event with no one present can have consequences that compound with every hour before help arrives.
Home can be made genuinely safe with the right modifications, the right support, and the right oversight. But the assumption that home equals safe, without those things in place, is a myth that leaves real vulnerabilities unaddressed.
Myth 3: Family Care Is Always Better Than Professional Care
This myth comes from love, and that is precisely what makes it so difficult to examine honestly.
The belief that a child’s care, given with genuine devotion, is inherently superior to anything a professional can offer is deeply embedded in Indian family culture. It is also, in important ways, not true.
Love is not the same as skill. A devoted family member who does not know how to safely assist a parent with Parkinson’s through a freezing episode can cause a fall. A well-meaning child who does not understand the medication interactions in a parent’s post-stroke regimen can inadvertently create a dangerous situation. A family caregiver who has no training in dementia communication may, with the best intentions, respond to their parent’s confusion in ways that increase agitation and distress.
Professional caregivers bring knowledge, training, and experience that love alone cannot substitute. They know how to observe clinical changes and escalate them appropriately. They know how to support rehabilitation goals. They know how to manage the specific behaviours and risks associated with conditions that require more than devotion to handle well.
The most effective care arrangements combine both. Family love and presence alongside professional skill and structure. One does not replace the other. They are designed to work together.
Myth 4: Ayurvedic and Home Remedies Can Replace Conventional Medicine
India has a rich and genuinely valuable tradition of Ayurvedic and natural medicine. Many Ayurvedic approaches have real evidence behind them for specific conditions, and integration of traditional practices with conventional medicine is a thoughtful approach that many clinicians support.
What the evidence does not support is replacement.
For chronic conditions common in elderly Indians, including diabetes, hypertension, Parkinson’s disease, and post-stroke care, conventional medication is not optional. It is the clinical foundation on which everything else rests. Levodopa for Parkinson’s, antihypertensives for blood pressure, anticoagulants post-stroke, these medications exist because the evidence for their effectiveness is substantial and well-established. Discontinuing or reducing them in favour of Ayurvedic alternatives, without medical supervision, carries serious and sometimes irreversible risks.
The myth that natural equals safe and pharmaceutical equals harmful is particularly dangerous in elderly adults, whose conditions are often more fragile and whose margin for error is smaller. Some Ayurvedic preparations interact with conventional medications in ways that affect efficacy or safety.
The right question is not whether to choose Ayurveda or conventional medicine. It is how to use both intelligently, transparently, and under medical supervision.
Myth 5: If They Are Eating and Moving Around, They Are Fine
This myth feels like common sense. A parent who is eating their meals and walking around the house appears to be managing. What more do you need to know?
Quite a lot, as it turns out.
Eating and moving are necessary conditions for well-being, but they are far from sufficient indicators of it. A parent can be eating meals while consuming inadequate protein, insufficient hydration, and not enough of the specific nutrients their body needs to maintain muscle mass, bone density, and cognitive function. A parent can be moving around the house while managing chronic pain that has gone unreported, navigating mobility limitations that are quietly worsening, and avoiding certain areas of the home because they do not feel safe in them.
This myth also misses the dimensions of well-being that are not visible in a video call or a short visit. Depression. Social isolation. Anxiety. Cognitive decline in its early stages. Chronic pain that a stoic parent does not mention because they do not want to worry you. These conditions do not announce themselves through appetite and ambulation.
Asking whether your parent is eating and moving is a starting point, not an assessment.
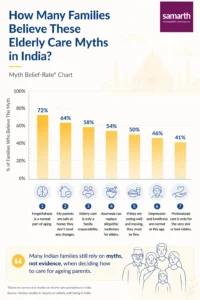
Myth 6: Depression and Anxiety Are Normal in Old Age and Cannot Really Be Treated
Depression and anxiety are common in older adults. They are not, however, normal in the sense of being inevitable, acceptable, or untreatable. This distinction matters enormously for how families respond when they see these conditions in their parents.
Depression in elderly adults is frequently missed because it does not always present the way families expect. It may look like withdrawal, fatigue, reduced appetite, and loss of interest in previously enjoyed activities rather than overt sadness. In India, where mental health carries significant stigma and where this generation of elderly adults was raised with no cultural framework for identifying or discussing psychological distress, depression often goes completely unnamed and therefore completely unaddressed.
The consequences of untreated depression in elderly adults extend well beyond mood. Depression is associated with faster cognitive decline, reduced immune function, poorer outcomes from physical health conditions, and significantly reduced quality of life. It is also associated with increased mortality.
Depression in older adults responds well to treatment, both psychological and pharmacological, when it is properly identified and addressed. The myth that it is simply part of getting old functions as a reason not to seek that treatment, and the cost of that inaction is real and measurable.
If your parent seems persistently withdrawn, disinterested, or flat in affect, a conversation with their doctor is the appropriate response, not acceptance.
Myth 7: Professional Care Is Only for the Very Sick or Very Old
This myth is perhaps the most limiting of all, because it delays care until a crisis makes it unavoidable.
The belief that professional care is a last resort, something you turn to only when a parent can no longer manage basic functions, means that families wait until their parent has had a serious fall, a significant health event, or a cognitive decline that has become impossible to ignore. By that point, the care needed is more intensive, more expensive, and harder to put in place well under time pressure.
Professional elder care works best when it is introduced gradually, before a crisis, as a layer of support that preserves independence rather than replacing it. A companion caregiver who assists with errands, monitors medication, accompanies a parent to medical appointments, and provides social engagement is not a sign that your parent has declined to the point of needing care. It is a sign that your family is being thoughtful about preventing that decline.
The parents who maintain the best quality of life in their later years are typically those whose families introduced appropriate support early, before circumstances forced the decision. Waiting for the crisis is not caution. It is a missed opportunity.
What Evidence-Based Elder Care Actually Looks Like
Evidence-based elder care begins with an honest assessment of where your parent actually is, not where you hope they are or where the myths suggest they should be.
It takes memory changes seriously and pursues diagnosis rather than reassurance. It modifies the home environment based on specific, identified risks rather than assuming familiarity equals safety. It combines family presence and love with professional skill and structure, understanding that these are complementary rather than competing. It manages chronic disease with the rigour it deserves, integrating traditional approaches thoughtfully and transparently under medical supervision. It monitors nutrition, hydration, and daily functioning as active responsibilities rather than background assumptions. It treats depression and anxiety as real conditions with real treatments. And it introduces professional support early, as an investment in independence, rather than waiting for a crisis to make the decision unavoidable.
This is the standard Samarth holds itself to, and the standard we believe every elderly parent in India deserves.
At Samarth, our care coordinators begin every engagement with a thorough assessment that looks honestly at your parent’s physical, cognitive, emotional, and social needs. We do not tell families what they want to hear. We tell them what their parent actually needs, and then we help them build the care to meet it.
For NRI families managing this from abroad, that honesty is not just reassuring. It is the foundation of every good decision you will make about your parent’s care.
The Most Loving Thing You Can Do Is Know the Truth
The myths in this blog are not held by careless families. They are held by devoted ones, people who love their parents and are doing their best with the beliefs they inherited and the information they have.
But love without accurate information can lead to decisions that feel right and work out badly. And your parent deserves better than decisions made on the basis of what everyone has always believed.
Replacing myth with evidence is not a clinical act. It is an act of love. It is choosing to see your parent clearly, to understand what they are actually experiencing, and to build care that responds to reality rather than assumption.
That is where good care begins. And it is never too early to start.
Beliefs about ageing should not be the basis of care decisions. Evidence should.
Samarth helps NRI families cut through assumptions and understand exactly what their parent needs, based on a thorough, honest assessment of where they actually are.
See What Professional Care Actually Looks Like







